
Keith Ayoob, EdD, RDN, FAND —
The latest statistics from the Centers for Disease Control indicate that 9.4% of the US population – more than 1 in 11 persons – has some form of diabetes.
The most common types of diabetes are called “type 1” and “type 2”. Type 1 usually emerges in childhood and is also called “insulin-dependent” diabetes, because the body’s pancreas malfunctions and produces little or no insulin.
More than 90% of diabetes however, is type 2, in which the body still produces insulin, but not enough to reduce blood glucose to normal levels in a reasonable amount of time, if at all.
As troubling as the statistics on diabetes are, more than 1 in 4 Americans has “pre-diabetes” — where blood glucose levels are often higher than normal but not high enough to be considered full-blown diabetes. Without any intervention, pre-diabetes is likely to transition into type 2 diabetes. However, with proper intervention, this transition to diabetes can be prevented or delayed. At the same time, most people with pre-diabetes don’t seek out medical advice or support for their pre-diabetes because they don’t even know they have it.
How does someone become pre-diabetic?
Genetics play a role, but so does family history of diabetes or simply being overweight or obese. Poor diet and having a sedentary lifestyle play important roles as well. Pre-diabetes is also tied to other silent health conditions, such as metabolic syndrome, hypertension and high blood cholesterol levels.
Does sugar “cause” diabetes?
No. But eating too much sugar can aggravate the condition by forcing your body to work extra hard to lower your blood glucose levels.
Does obesity cause diabetes?
Here things get more tricky. Obesity doesn’t directly cause diabetes, but it can cause “insulin resistance”. Having excess body fat can cause your cells to react differently to the insulin your body puts out. Insulin resistant people react LESS to the same amount of insulin that they did before they gained weight. As a result, your body has to produce more and more insulin to keep blood glucose levels under control. Eventually, even those higher levels of insulin just don’t do the trick, and blood glucose stays high. Then you’re either prediabetic or diabetic.
Prevention is where nutrition, diet, and lifestyle have their greatest impact. If you have pre-diabetes, the good news is that you’re at a “fork in the road” — you still have a chance to determine your direction.
Overweight or obesity usually accompany pre-diabetes, so losing weight is key, but you don’t need to lose massive amounts of weight to get healthier. Losing as little as 5% of your weight (think 10 pounds if you’re 200 pounds now) can be enough to bring blood glucose levels under control. Keeping it under control also requires some tweaks to your diet and lifestyle so you don’t regain the weight and perhaps approach an even healthier weight.
Gradually becoming more physically active can go a long way towards managing your blood glucose level. There’s no need for extreme activity, but a 20-minute brisk walk on most days can not only help with weight management but helps prevent spikes in blood glucose.
Even being “less sedentary” throughout the day helps. Taking the stairs when you can, parking further away from the store, and going to pick up your lunch instead of having it delivered, can get you moving and prevent your metabolism from slowing down.
Most people eat too much added sugar. As you can see here, beverages are the largest source of added sugars, followed by snacks and sweets like candy:
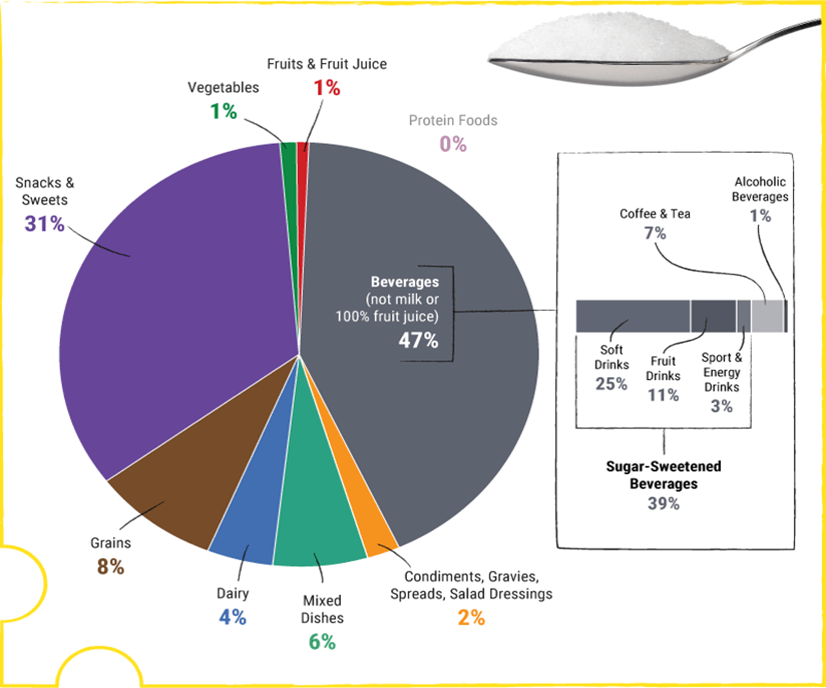
Data Source: What We Eat in America (WWEIA) Food Category analyses for the 2015 Dietary Guidelines Advisory Committee
Using LCS is an ideal way to replace most or even all the added sugars in beverages. According to the above graph, doing so would reduce our added sugars by a whopping 47%!
It’s also key to look at where we are drinking those beverages. The CDC determined that slightly more than half (53%) of our consumption of sugar-added beverages are consumed at home, the rest away from home:
Drink At Home (53%) Drink Away From Home (47%)
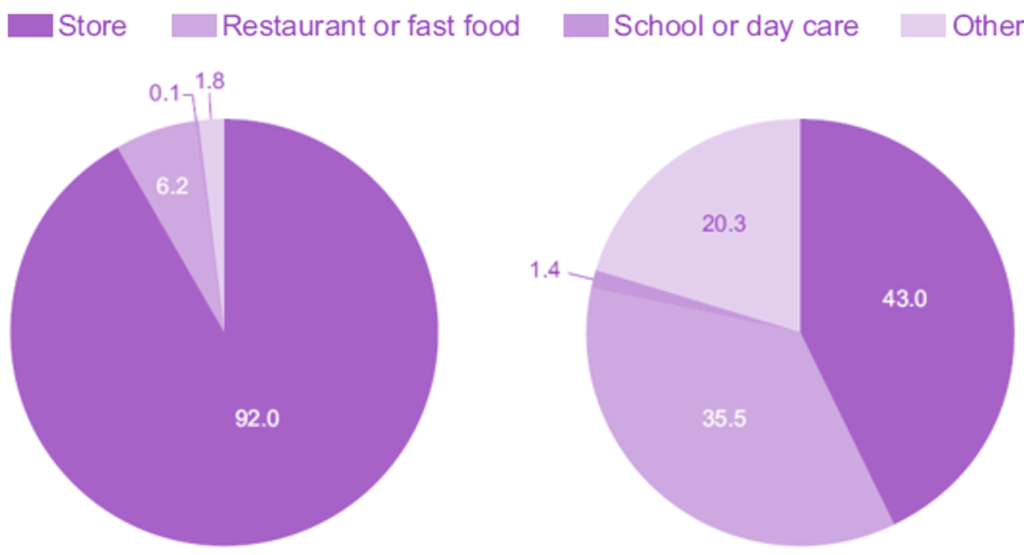
Source: NCHS Data Brief No. 71, Figure 6. August 2011
Whether we’re home or away, we can do a lot to reduce the added sugars in our diets, help manage our blood glucose levels, and reduce the amount of “empty calories” we eat.
It’s not just about beverages though. LCS can also reduce the added sugar in many nutritious dairy foods like yogurt, allowing us to get great taste and nutrition with fewer calories.
The true cause of obesity is EXCESS – whether that excess comes from sugar, total calories, or excess inactivity. LCS are great tools for reducing one of those excesses: added sugar. And they can be useful to pre-diabetics or anyone who desires less added sugar.
Data Source: What We Eat in America (WWEIA) Food Category analyses for the 2015 Dietary Guidelines Advisory Committee

Keith Ayoob, EdD, RDN, FAND, is an Associate Clinical Professor Emeritus at the Albert Einstein College of Medicine. As a pediatric nutritionist and registered dietitian, Dr. Ayoob is also a past national spokesperson for the Academy of Nutrition and Dietetics. Dr. Ayoob is a consultant with the Calorie Control Council Advisory Board and the Global Stevia Institute (GSI), GSI is supported by PureCircle Ltd, a global leader in purified stevia leaf extract production.